

Success Stories
"Each and every nurse was extremely wonderful!"
Terry
Admitting Diagnosis: Acute on chronic hypoxic respiratory failure with mechanical ventilation, non-Hodgkins Lymphoma, Acute Kidney Injury, Pneumonia, deconditioning and malnutrition.
Length of Stay: 35 days
Referring Facility: University Hospitals Cleveland Medical Center
Discharge Destination: SNF
Discharge Date: 10/10/25
Terry presented to UH Parma Medical Center due to recurrent falls at home, generalized cancer pain, and electrolyte imbalance. During his admission, his breathing condition declined, he became confused, and his vital signs became critical. He was transferred to UH Cleveland Medical Center where a tracheostomy and ventilator became necessary; he was dependent for all care.
Terry was admitted to Grace Hospital 9/5/25 with acute on chronic respiratory failure with mechanical ventilation, pain related to non-Hodgkins Lymphoma, AKI, Pneumonia, deconditioning and malnutrition. He was dependent for all care.
Following his 35 days stay at Grace with nutritional support; physical, occupational and speech therapy; daily physician and pulmonary visits; and nursing care, Terry made significant improvements. He was able to walk with a wheeled walker 50-65' and moderate assistance, his standing tolerance improved, and his activities of daily living improved to requiring minimal to moderate assistance for upper body care.
He said it may take some time, but he plans to return to the unit with his homemade spaghetti and meatballs for the staff. His brother wanted to thank the staff for taking such good care of his brother.
"My wound nurse is wonderful. My skin looks amazing! I don't want to leave."
Joanne

Admitting Diagnosis: Cellulitis, sepsis, peripheral artery disease, endocarditis, lower leg worsening, open wounds
Length of Stay: 25 days
Referring Facility: Cleveland Clinic Medina Hospital
Discharge Destination: UH Parma Acute Rehab
Discharge Date: 10/3/25
Joanne presented to Medina Hospital due to worsening lower extremity wounds that she had for "years" and were becoming painful and making it difficult to walk. Joanne was admitted to Grace Hospital 9/8/25 with bilateral lower leg open wounds with daily treatment, IV antibiotics for infection, and required maximum assistance for mobility and moderate to maximum assistance for activities of daily living.
Admit
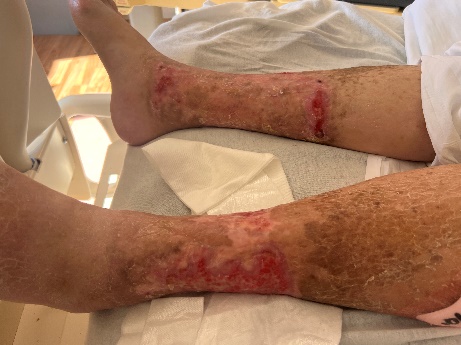
Discharge
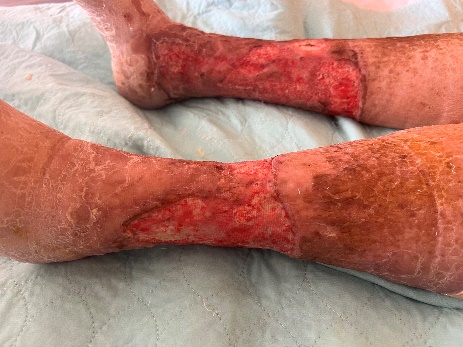
Following her 25 days stay at Grace with daily wound care, a protein rich diet, physical and occupational therapy; Joanne is now able to walk with a wheeled walker 80-90' and minimal assistance. Her activities of daily living improved to requiring stand by assistance for upper body and moderate assistance for lower body.
She discharged to UH Parma Acute Rehab to continue her recovery and gain more independence.
John
Admitting Diagnosis: Acute Respiratory Failure with mechanical ventilation, epilepsy, chronic thrombocytopenia, and metabolic/hepatic encephalopathy
Length of Stay: 36 days
Referring Facility/Physician/CM: University Hospitals, Elyria Memorial Medical Center, Dr. Ahmed Darwish, Case Managers Elizabeth and Brigid
Discharge Destination: Skilled Nursing Facility for additional therapy with the goal to transition home.
John is a 60-year-old admitted from Elyria Memorial Medical Center ICU, where he spent 18 days prior to admission. When he arrived, he was dependent on the ventilator to breathe, required a tube feeding for nutritional support, and was dependent for all care and activities of daily living.
During his stay, John was able to progress to having the tracheostomy tube removed and eating a regular diet. He was able to walk with a walker 150-200' and walk up and down 5 steps with a rail. He was able to perform activities of daily living with stand by to minimal assistance. John stated he enjoyed laughing with the staff at Grace Hospital.
When asked about his progress, John's sister, Cindy, stated, "John has come a long way. It's wonderful to see him up and moving. I see a big, big difference. Wonderful job Grace!"
"The minute we entered the unit, we said this is the place! We saw the nurses in the rooms caring for the patients! We chose Grace because of the amazing nursing care."
Bonnie
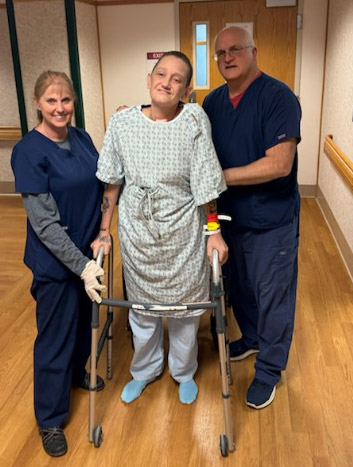
Admitting Diagnosis: Acute respiratory failure, traumatic brain injury status post craniotomy
Length of Stay: 27 days
Referring Facility: Metro Health, SW: Rachel Medvetz, Physician: Dr. Curley
Discharge Destination: Metro Health Traumatic Brain Injury Program
Discharge Date: 2/12/25
Bonnie is a 39-year-old patient who presented to Metro Health with a subdural/subarachnoid hemorrhage following a seizure and hitting the back of her head. She was admitted to Trauma ICU with worsening symptoms requiring a craniotomy, tracheostomy and ventilator, peg feeding tube, and critical drips to maintain normal vital signs. She was able to be weaned off of the critical drips and the ventilator prior to transfer to the long-term acute hospital.
Bonnie was admitted to Grace Hospital 1/16/25 with a trach collar and peg tube, did not show any response to voice or movements, and was dependent for all care.
Following her 4 weeks stay at Grace, Bonnie is now able to walk with a walker and minimal assistance, her trach was removed, she was upgraded to a regular diet, and is able to interact and joke with staff. She will be discharging to Metro Health Traumatic Brain Injury Program to continue her recovery and gain more independence.
Her mother, Barbara, has been by her side the entire stay and can't believe her progress. She was thrilled to have Bonnie's journey highlighted as a Success Story at Grace. When asked why she chose Grace Hospital, she stated, "My son and I came unannounced to tour the facility. The minute we entered the unit, we said this is the place! We saw the nurses in the rooms caring for the patients! We chose Grace because of the amazing nursing care. You not only treated Bonnie, but you also treated us, the family. Asking us, how are you doing and can we get you anything? We knew Bonnie was getting cared for and this allowed us to comfortably go home. This is an amazing place!"
"The physical therapists and medical staff at Grace were great. They took the time to actually understand me and how difficult it was for me to go through this, having been entirely healthy before the accident."
When a person hears "long-term acute care," one generally envisions the patients as being of elderly age – a common misconception. That wasn't the case for M.L., who at the young age of 20 was transferred to Grace Hospital following a tragic motor vehicle accident involving a semi truck.
When she arrived at Grace Hospital, her list of medical traumas was lengthy and complex, including bilateral pneumothoraces, a traumatic brain injury, a lacerated liver and spleen, a shattered pelvis with an external fixation, and multiple other fractures. As a result of the crash, she developed acute respiratory distress syndrome (ARDS), which occurs when fluid builds up on the lungs, causing oxygen deprivation.
To treat her complex injuries, bilateral chest tubes were placed and tracheostomy and PEG tubes were inserted for feeding purposes.
"I was transferred to Grace after being in a medically induced coma for three weeks," said the patient. "Grace, by far, had the best ratings for ventilator weaning, so we were hopeful."
While at Grace, the patient received an integrated treatment approach involving critical care medicine, ventilator weaning, and physical and occupational therapies.
"I had to relearn how to walk again," said the patient. "The physical therapists and medical staff at Grace were great. They took the time to actually understand me and how difficult it was for me to go through this, having been entirely healthy before the accident." Today, she is healthy and thriving. Although she's still recovering from a traumatic brain injury and pelvis pain from the semi truck's impact, and has returned to both school and work.
"Everyone at Grace was always looking out for me in any way they could as I was regaining my independence," said the patient. "I've been back to visit, and they're still always so caring and welcoming."
I want others to know that Grace Hospital exists. Not having to move my dad around and having everything he'd need to ensure his comfort in his final days was truly a blessing. We're so grateful.
When Norman, 88, arrived at the Bedford Intensive Care Unit in late March, his disease had progressed to a point where there was little doctors could do to help, except provide him with comfort and hospitality during his final days.
Suffering from an acute case of Emphysema, a form of Chronic Obstructive Pulmonary Disease (COPD) in which the lungs becomes irreversibly damaged, causing an obstruction in air flow, Minihan was transferred to Grace Hospital, an acute care hospital specializing in providing care for patients with highly complex medical conditions.
"When we first arrived at Grace, it was like this hidden gem. It was on a different floor of the Bedford ICU, and it was just so private and quiet," says Louise Sansom, Norman's daughter. "The staff was just incredible. On our second day there, they knew all of us by name – and there were a lot of us!"
As the disease continued to take a toll on his already frail lungs, Norman's family became worried they would have to move him to a hospice facility. To their relief, a doctor assured the family that Grace Hospital could care for all of Norman's medical needs without him ever having to move.
"Grace was like a one-stop shop for us. My dad never had to ask for anything – there was always someone nearby to help," says Sansom. "We felt so much compassion from each and every staff member, from the people who brought his food, to his doctor. They were always checking on us and making sure we had everything we could possibly need."
Even after Minihan passed away just two weeks later, Sansom says she recalls seeing some of the staff members crying behind the nurses' station.
"After being in this field for years, people tend to grow cold and apathetic to death. But that wasn't the case at Grace at all," says Sansom. "It was obvious they really, truly cared for my dad."
Having been deeply touched by the care Minihan received at Grace, his family decided to donate any memorial contributions to Grace Hospital, in lieu of flowers.
"I want others to know that Grace Hospital exists," says Sansom. "Not having to move my dad around and having everything he'd need to ensure his comfort in his final days was truly a blessing. We're so grateful."
"I needed a new liver to save my life, but I needed the right kind of care to make a full recovery and thrive."
Hepatopulmonary Syndrome (HPS), which affects individuals with an existing liver disease, is an uncommon condition in which the lung's blood vessels expand, making it difficult for the lungs to absorb enough oxygen. The only cure is to have a liver transplant.
"When I was diagnosed in May 2013, doctors told me I wasn't going to live past Christmas," says Brian, a recent liver transplant recipient. "By the time I received my new liver, I was in pretty bad shape. My lungs were severely damaged, and I couldn't move."
Following the operation, just two days before Christmas, Brian was admitted to Grace Hospital, a long-term acute care hospital specializing in providing care for patients with highly complex medical conditions. Dependent on 15 liters of oxygen daily, his oxygen levels would drop by 30 percent just from sitting up in bed.
"It was going to be a slow recovery, and everyone knew it," says Brian. Utilizing an integrated treatment approach of critical care medicine, pulmonology, nursing, respiratory therapy, physical therapy, occupational therapy, clinical pharmacology, nutritionist and case managers, Grace Hospital's interdisciplinary team of physicians and specialists helped Brian regain his health and quality of life.
"Everyone was there because they wanted to see their patients have a successful outcome," says Brian. "Every day, they pushed me to get up and walk. They told me it'd be baby steps at first, but they had faith one day I'd be walking without oxygen. They never took 'no' for an answer."
Now, just three and a half months after being discharged from Grace Hospital, Brian is down to only 5 liters of oxygen per day while walking and only 1.5 liters of oxygen at rest. Over the next several months, he's expected to no longer need breathing assistance. He attributes his success to the quality, hands-on care he received at Grace Hospital. "I needed a new liver to save my life, but I needed the right kind of care to make a full recovery and thrive," says Brian. "In the absence of Grace Hospital's care, the new liver wouldn't have mattered."
"Winning the wrong lotto - twice!"
- Richard R, Garfield Heights, OH
Guillain-Barre (pronounced Ghee-lan Bar-ray) Syndrome (GBS), a rare disorder in which the body's immune system attacks part of the peripheral nervous system afflicts only 15 people per million per year in the United States. And of those, only 3% may suffer a relapse of muscle weakness and tingling sensations many years after the initial attack.
"I was told the odds of aquiring GBS again are so small it would be like winning the lottery twice," says Richard Rossi, a dedicated lotto player and victim of the chronic form of GBS. "Some lottery!"
When Richard entered Grace Hospital, a long-term acute care hospital which specializes in providing care for patients with highly complex medical conditions, he was battling pneumonia and infections and breathing with the assistance of a ventilator.
Grace Hospital's Interdisciplinary Team of physicians and specialists -- in the fields of neurology, critical care medicine, pulmonology, nursing, respiratory therapy, speech therapy, occupational therapy, clinical pharmacology, and social work -- combined their medical expertise to help Richard fight his illness and regain his quality of life.
Through personal perseverance and excellent medical support, Richard's condition dramatically improved. He was successfully discharged from Grace Hospital and has returned to his daily activities.
"I wanted to return to my family and continue doing what I enjoy," says Richard. "Grace Hospital's integrated approach to my care - and continual communication with my family and me - helped me get where I am today."
Amazingly, his luck continues. He recently sunk a hole-in-one on the golf course. At least this time it is positive luck!
"I want to show them what I've been able to accomplish through their unique approach. I am their success."
-Daniel P
It is a hospital visit he remembers little about, but Daniel does know that when he left Metro Health Hospital, he was a very sick man and ventilator dependent. As Daniel's wife, Virginia says, "He had a coronary artery bypass graph and during surgery his heart had to be shocked back into rhythm twice and his body shut down; his kidneys failed, dialysis was required and he was unconscious for four and a half weeks. At that time, I was told that he needed to be moved to a hospital that would be able to give him the care he needed."
Grace Hospital at Fairview was Virginia's first choice for her husband because, "It is such a bright, cheery looking place that to me if you are a patient and open your eyes and see you're in this lovely looking room it does so much more for you to be able to get better. They are also expert at treating extremely sick patients and providing very personal care." Dr Neal Chadwick, Medical Director of the LTACH, Grace Hospital Long-Term Acute Care Hospital, and a pulmonary specialist describes the difference between an LTACH and ICU as, "An ICU is like a sprint and the LTACH as a marathon. We tend to have a long term approach to patients whereas an ICU has a crisis approach."
Ventilator weaning is a specialty of Grace Hospital, which employs a different approach, a TIPS protocol. As Chadwick explains, "This is short for Therapist Initiated Patient Specific and what it does is establish a set of parameters to use on these patients. It allows the therapist to wean the patient when we are not even present. They measure volumes, pressures and the way the patient is behaving on the ventilator and the therapist can change the ventilator to fit the patient's needs. We tend to wean much more quickly than they do in the Intensive Care Unit, where the physician makes changes once a day, because here with the TIPS protocol, we can wean around the clock." Although Virginia did not initially believe it would be 24 hour weaning, she learned it is. "They work with the patient 24 hours and sometimes they'd wean him down and then they'd see he was having a problem and they would work him back up again so he was not finding it as difficult to breathe. It is excellent care." Daniel did not even know that he was breathing on his own. "When they shut the ventilator off, they never told me for hours and hours. After twelve hours of breathing on my own, they told me the ventilator was not assisting me. I didn't even realize it, because they do it so gradually and around the clock."
When Daniel no longer needed the specialized treatment that Grace Hospital provides, the transition to Fairview Hospital Rehabilitation Unit to continue with physical therapy and nutritional care was easy as Daniel says, "I just had to go down in an elevator to Fairview Hospital, where, over time, I learned to walk and eat. And although I was no longer at Grace Hospital some of the people who worked with me there came to visit."
"Grace is unique," according to Daniel, "they explain to the family and patient what is going on. They always come to chat, even when I couldn't talk back. From the doctors, nurses, therapists, aides and even cleaning staff, everyone shows how much they feel for you by maintaining a positive, encouraging attitude. They sincerely care."
Though he didn't know he arrived at Grace Hospital due to the severity of his illness, now that Daniel is well on the road to recovery he wants to visit his caregivers there. "I want to show them what I've been able to accomplish through their unique approach. I am their success."
About Grace Hospital
Our mission is to serve as a center for excellence in the provision of specialized health care services and comfort for patients and families coping with catastrophic illness and injury.
216-687-1500
2307 West 14th Street
Cleveland, OH 44113
